Body
Article summary:
- Two new studies exploring respiratory muscle weakness — specifically about the diaphragm muscle, an essential muscle for breathing — have implications for both clinicians and patients.
- One study finds the causes and recovery patterns of phrenic neuropathy (PhN) among patients in outpatient rehabilitation.
- Another finds that the use of diaphragm ultrasound in inpatient rehabilitation care is a predictor of successful ventilator weaning after a spinal cord injury.
Clinicians and scientists at Shirley Ryan AbilityLab are leading new research to expand understanding of respiratory muscle weakness and the diaphragm — a critically important muscle for breathing — in two new studies published in peer-reviewed journals. The research has implications for clinicians to create more effective treatment plans, set precise rehabilitation goals and help patients reach improved outcomes as they recover from impairments to their breathing.
Study Identifies Phrenic Neuropathy (PhN) Causes
Body
In a benchmark study published in Muscle & Nerve, researchers explore the causes and recovery patterns of phrenic neuropathy (PhN). PhN is a condition affecting the phrenic nerve — the vital nerve that controls the diaphragm and facilitates breathing. PhN impairs diaphragm function, which can cause a spectrum of breathing issues, including shortness of breath, difficulty sleeping or exercising, and recurrent pneumonia. In the most severe cases, patients with PhN may require mechanical ventilation.
Despite the significant impact of PhN, its causes have been ill-defined, which may impact clinicians’ ability to develop effective treatment plans for patients.
“In this study, we wanted to better understand the knowledge gaps around PhN — its causes, outcomes and recovery patterns — especially in a clinical rehabilitation practice, including referrals to our outpatient rehabilitation and neuromuscular medicine clinics,” said Colin Franz, MD, PhD, a physician-scientist at Shirley Ryan AbilityLab who is one of the authors of the new study. “This research is especially timely, as the incidence of PhN appears to be on the rise due to COVID-19 and its associated effects on the respiratory system.”
The study included 151 patients who were treated for PhN at two interdisciplinary clinics and followed by neuromuscular-trained neurologists or physiatrists. Their recovery from PhN was evaluated using various inputs, including pulmonary function tests, diaphragm muscle ultrasound and patient self-reporting.
The researchers found the most common causes of PhN: 27% of cases are idiopathic, or spontaneous; 24% are associated with cardiothoracic procedures related to the heart, lungs and chest; and 17% follow a stay in an intensive care unit — including COVID patients and others.
Also, the majority of patients with PhN regain diaphragm muscle function, but on average it takes 15 to 17 months for patients to see improvements — an insight from the research that can inform the optimal timing for specific pulmonary rehabilitation interventions.
“Having a better understanding of the causes of PhN, as well as the length of time it may take a patient to recover, will help improve how we treat patients to regain function of their diaphragm muscle and, hopefully, experience easier breathing,” said Dr. Franz.
Furthering the study of PhN, Dr. Franz recently received a grant from the National Institutes of Health (NIH) to develop therapeutic electrical stimulation for patients with PhN. Using wireless, bioresorbable implants, the new therapy aims to accelerate diaphragm muscle function in patients with PhN faster and more completely than ever before.
Additionally, Dr. Franz recently was recruited to establish a dedicated Diaphragm Muscle Clinic at the Northwestern Medicine Canning Thoracic Institute, alongside Northwestern’s Lisa Wolfe, MD, and John Coleman, MD.
Diaphragm Muscle Ultrasound Predicts Ventilator Weaning Outcomes
Body
While the Muscle & Nerve research studied the diaphragm muscle in people in an outpatient rehabilitation setting, the second research paper focuses on inpatient care — specifically investigating the use of diaphragm muscle ultrasound to predict ventilator weaning outcomes after a cervical spinal cord injury (SCI), which is a severe SCI high on the spinal cord. The study will be published in the Journal of Ultrasound in Medicine, and was led by Shirley Ryan AbilityLab’s Natasha Bhatia, MD, and co-authored by Dr. Franz and other clinicians from the rehabilitation hospital.
Body
When patients experience respiratory failure after SCI, they may need to rely on a mechanical ventilator to help facilitate their breathing. Over time, physicians seek to wean patients off ventilators so they can breathe independently, continue their recovery and have an improved quality of life — and to reduce the risk of serious infections like pneumonia and of shorter life expectancy that comes with being dependent on ventilators.
In fact, Shirley Ryan AbilityLab has pioneered a novel approach to ventilator weaning — an early, proactive intervention in which patients receive targeted muscle training to strengthen all of the muscles used for breathing and learn techniques that help increase the efficiency of their breathing.
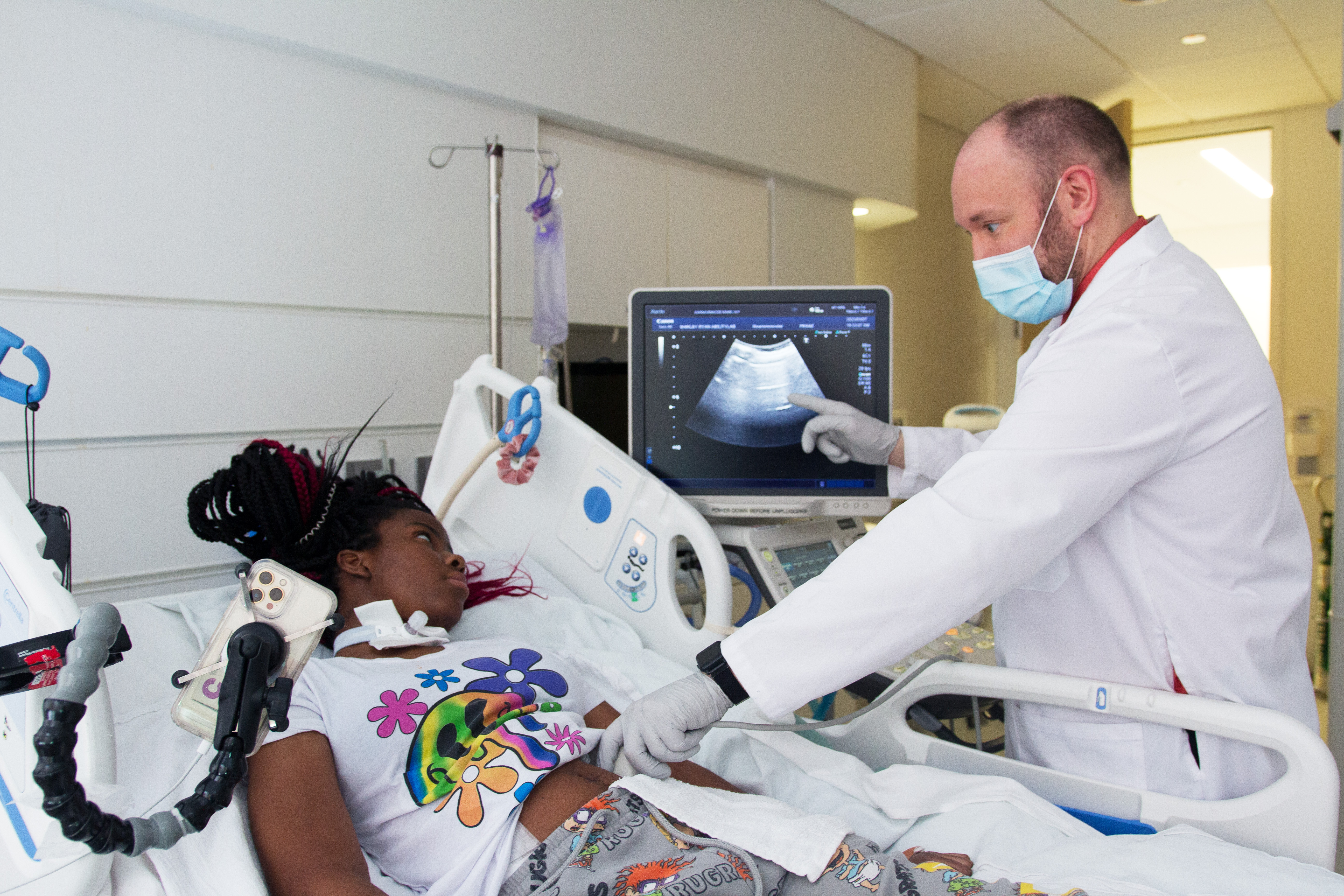
This latest research is a retrospective case series looking at patients with SCI who were dependent on a ventilator when they were admitted for inpatient rehabilitation. In the 21 patients enrolled in the study, a diaphragm muscle ultrasound had been performed to measure the thickness of the diaphragm and the thickening ratio, which impacts the diaphragm’s ability to contract.
Of the various measurements taken by the ultrasound, the researchers learned that the thickening ratio was the best predictor for ventilator weaning outcomes and predicting the muscle’s readiness to benefit from respiratory muscle training and exercise in rehabilitation. When diaphragm contractions were in a normal range, it was an indicator that a patient may successfully be liberated from a ventilator by their target discharge date from inpatient care and build back diaphragm muscle strength and endurance through rehabilitation.
“By using the measurements from a diaphragm muscle ultrasound, physicians will be able to set more precise rehabilitation goals for our patients, helping them to wean from a ventilator and continue recovery with ventilator-free breathing and an improved quality of life,” said Dr. Franz.