Body
Guillain-Barré syndrome (GBS) is a rare neurologic condition in which a person’s immune system attacks their own nerves — causing muscle weakness and, sometimes, severe mobility, breathing and swallowing issues.
According to the U.S. Centers for Disease Control and Prevention, GBS affects 3,000 to 6,000 people in the United States every year. Fortunately, with treatment and rehabilitation, many patients can make full recoveries.
In the following Q&A, Shirley Ryan AbilityLab’s Leslie Rydberg, MD, provides an overview of GBS causes and symptoms — as well as the important role of intensive rehabilitation in helping patients recover.
What is Guillain-Barré syndrome?
Body
GBS is a rare neurologic condition in which a person develops weakness, numbness and tingling that starts in the legs and feet and spreads its way up the body. It can lead to problems with walking and, in more severe cases, breathing and swallowing.
What causes Guillain-Barré syndrome?
Body
The nerves control the body’s muscles and send signals to the brain about pain, temperature and texture. However, in an individual with GBS, the nerves’ normal function is disrupted as the patient’s immune system attacks the nerves in the body. This is a type of peripheral neuropathy, which means that these signals are interrupted — leading to numbness, tingling and/or weakness.
Who is at risk of getting Guillain-Barré syndrome?
Body
The rate of GBS increases with age, although people of all ages can be affected. The overactive immune response in GBS can start after certain types of infections. Less commonly, it can be seen after getting a vaccine or with systemic conditions such as lupus, lymphoma or sarcoidosis.
What are common Guillain-Barré syndrome symptoms and when should people seek treatment?
Body
GBS symptoms typically progress quickly, within a few days to a few weeks. If someone develops foot weakness or experiences sensory changes that progress up the legs, they should go to the emergency department immediately for evaluation.
GBS can be a challenge to diagnose. Muscle problems, problems with the spinal cord, multiple sclerosis and other peripheral neuropathies can also cause leg weakness.
Once a patient has a GBS diagnosis, patients typically undergo IV treatment with intravenous immunoglobulin (IVIG) or plasma exchange. These treatments are very effective in stopping the immune system’s attack on the nerves.
How does rehabilitation help patients with GBS recovery?
Body
After initial treatment, the most important thing for patients to do is seek GBS rehabilitation. The attending physician in the acute-care hospital, or the patient’s general practitioner, may refer the patient to a rehabilitation hospital to continue their recovery in the inpatient or outpatient setting.
GBS rehabilitation can take many forms and include various clinicians:
- Speech-language therapists work on swallowing and cough strength.

- Physical therapists work on leg strength, getting in and out of bed, walking and using devices that can help with mobility. Additionally, they may offer aquatic therapy to help patients with strength, balance and stretching.
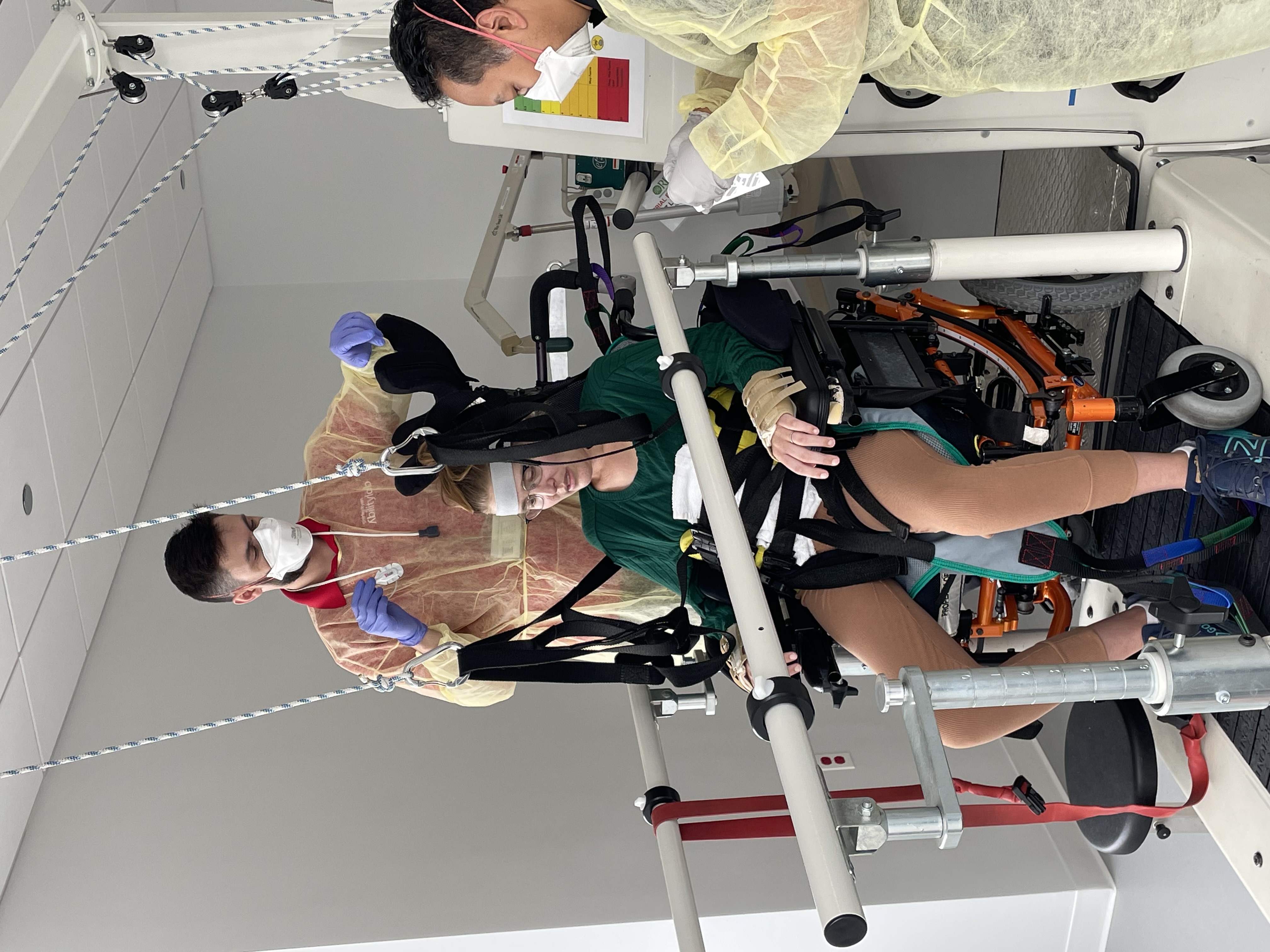
- Occupational therapists work on hand strength and activities like writing and eating. They also work on functional tasks like getting dressed and going to the bathroom.
- Orthotists design braces that can help patients compensate for arm or leg weakness.
- Art therapists can help patients work on hand coordination and dexterity through art and expression.

- Respiratory therapists work on cough strength and breathing support.
- Dieticians help patients get good nutrition so they have enough energy to participate in therapy.
- Psychologists work with patients to help them face the fear and uncertainty that can come with the diagnosis.
- Case managers help patients get access to the equipment and therapies that they need as they transition back into the community.
People who have more serious cases of GBS usually do best with treatment in an inpatient rehabilitation facility like Shirley Ryan AbilityLab. Afterward, they can benefit from continued intensive therapies, often in the DayRehab setting. People with less severe symptoms may be able to go straight to DayRehab for therapy. (Visit our blog to learn more about Rehabilitation Levels of Care.)
How does Shirley Ryan AbilityLab help patients with Guillain-Barré syndrome?
Body
Shirley Ryan AbilityLab is a great place for GBS recovery. Although it is an uncommon condition, we see a lot of patients with GBS and have a unique ability to care for those with more severe cases. We have an interdisciplinary care team, with expert therapists, nurses and physicians who are very knowledgeable and experienced in GBS treatment. Additionally, we leverage state-of-the-art equipment to ensure that people have the best possible chance of recovery. It is ideal to participate in a coordinated and intensive rehabilitation program — and we offer one.
Can people with Guillain-Barré syndrome make full recoveries?
Body
People with GBS can make full recoveries, but some people with more severe cases may continue to have some long-term muscle weakness. The recovery process can take as long as 12 to 18 months, so people often participate in therapies for an extended period of time or come back for additional therapy later.
People who are older, have severe breathing problems, and/or had a rapid onset of weakness may confront more challenges in their recovery. We support these patients in recovering some of their lost abilities and regaining as much function as possible.
Meet the Expert
Body
Leslie Rydberg, MD, is an attending physician at Shirley Ryan AbilityLab, as well as the Henry and Monika Betts Medical Student Education Chair and the Assistant Residence Program Director.
As a general physiatrist, Dr. Rydberg’s primary clinical interest is in neuromuscular disorders and medically complex rehabilitation. She also has a special interest in residency and medical student education, and holds roles as assistant professor of Physical Medicine & Rehabilitation and Medical Education at Northwestern University Feinberg School of Medicine.